Infarction of the spinal cord may present numerous symptoms that manifest dependent on the affected vascular area. According to research this is an uncommon disorder and has an estimated frequency of 0.003 percent of all incidents and 0.3-2 percentage of all stroke-related events [1,21.
Most of the time there is no etiology recognized. Causes can be categorized into iatrogenic and non-iatrogenic; the former may be due to aortic surgery or injuries caused by other surgical procedures, while non-iatrogenic causes include trauma, arteriosclerosis, arteriovenous malformations, thrombotic/fibrocartilaginous emboli, polycythemia vera, vertebral hyperextension, myelitis, infections, and/or neoplasms [1,3].
This case report seeks to provide a unique case with an acute spinal cord ischemia syndrome that has an unusual presentation and treatment, specifically the treatment and etiologic investigations.
An older 39-year old caucasian man with a history of cigarettes smoking, occasionally using cannabinoids, as well as hypertension, presented at the Emergency Department (ED) with an acute constrictive pain that was felt on the posterior side of the thoracic area beginning within an hour of admission radiating to the interscapular area and the upper limbs to the elbows, and an 8/10 severity of pain with no evidence of prior trauma.
When he was admitted to the ED the patient was diagnosed with an esophageal blood pressure of 192/113mmHg, the pulse rate was 130 beats/min, steady rhythm and temperatures of 36.8degC and the respiratory rate was fourteen breaths every minute. The physical exam was normal, with cardiac auscultation that was unmistakably clear and pulmonary auscultation that was normal, with no incidental murmurs, and there was no peripheral edema. The neurological exam revealed no deficits in the focal area. An electrocardiogram (ECG) revealed sinus rhythm, and ST depression in the leads V4-V6. Complete blood counts as well as base metabolic panel were in order without any elevation of inflammation variables (C-reactive Protein that was 3.2 mg/L) and no rise in biomarkers for cardiac health (troponin I, creatinine-phosphokinase, and myoglobin) between the hours of one and six. Furthermore, he was diagnosed with an natriuretic peptide B-type concentration of 43pg/mL. An echocardiogram of the transthoracic region was taken and revealed concentric, mild left ventricular hypertrophy with any other irregularities. To rule out an Aortic dissection, a computed tomography scan (angio-CT scan) of the abdomen, thorax as well as the pelvis (Figure 1.) was taken, revealing no sign of abnormality. Patient was admitted to hospital for observational clinical care due to the persistence of symptoms.
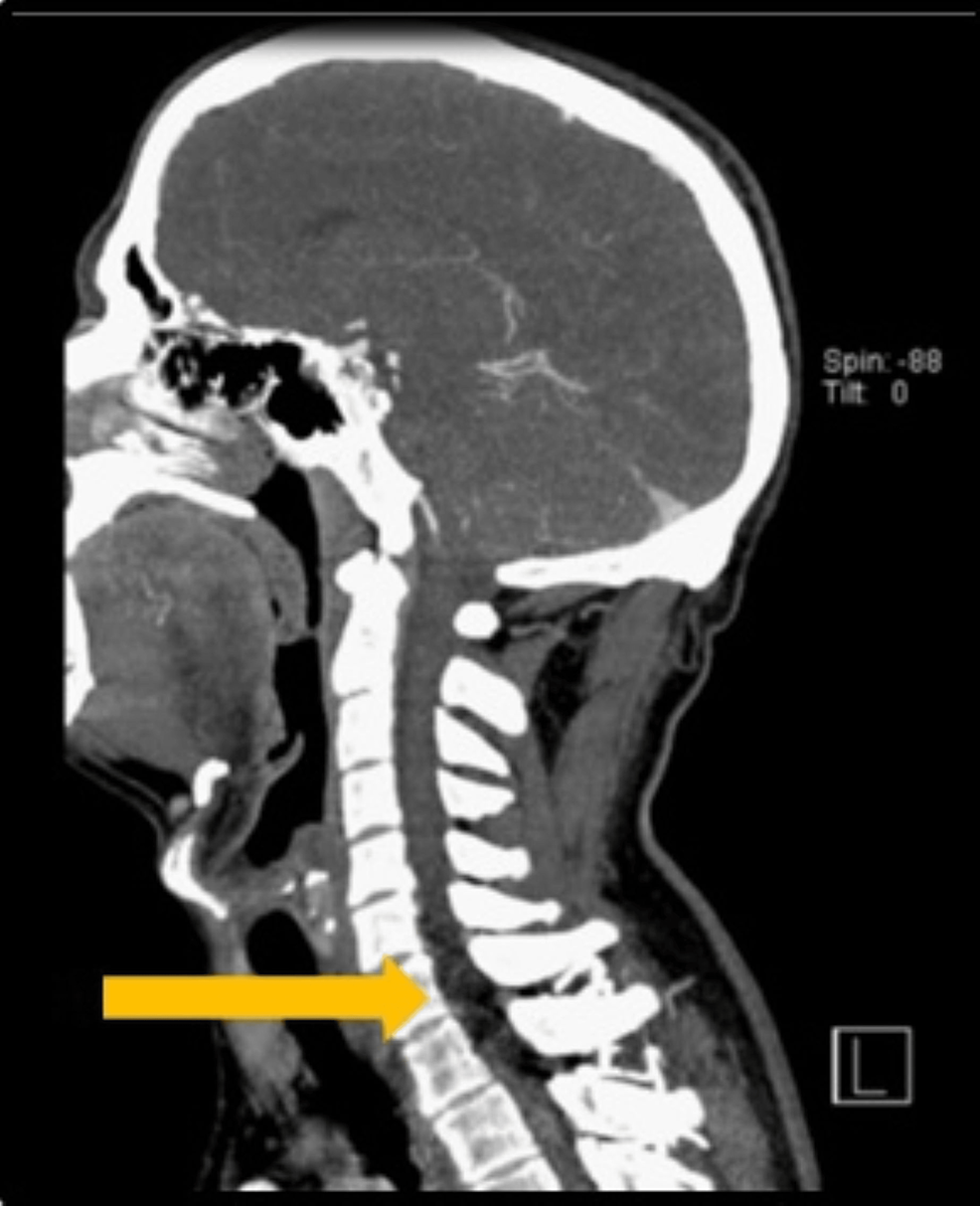
The following day, during being admitted to the hospital, the patient was found to show neurological signs and showed decreased strength in the lower leg of his left, as well as both hands, with decreased sensitivity in the area which corresponds to the dermatomes of T9-T12 that was linked to the acute retention of urine. The neurologic exam identified myotic pupil, a lack of photoreactive, difficulties in hand grip bilaterally with grade 3/5 muscle power in left lower limb reduced abdominal sensitivity below T5 in addition to bilateral hyporeflexia. Because of using morphine as a pain relief, naloxone was given without any an improvement in symptoms or physical exam results. A quick Angio-CT scan (Figure 2.) was conducted, which revealed the lesional region extending from C5 to the D2 region, mostly that affected the space between the left anterior and lateral suggesting an acute Ischemic spinal cord injury. Due to the subacute nature of the disease in the patient and an National Institutes of Health Stroke Scale (NIHSS) score of 3 this patient could not be subjected to thrombolysis or thrombectomy or both. The dual antiplatelet treatment (DAPT) as well as a high-potency statin were commenced. Electromyography done after five days after the first event showed increased the latency of F waves in both lower and upper limbs. These findings are likely to be related to involvement in the motor portion proximal that is part of the spinal reflex arc. Furthermore, there were signs of a mild neurogenic disorder that was not recent in the C7 region bilaterally, but without activation of the voluntary motor units in C8, and also bilaterally. Also, hyporeflexia of the upper limbs proximal to C7 as well as isoflexia of the lower limbs, and sensory levels at T3 was observed. In sum, these results indicated medullary dysfunction.
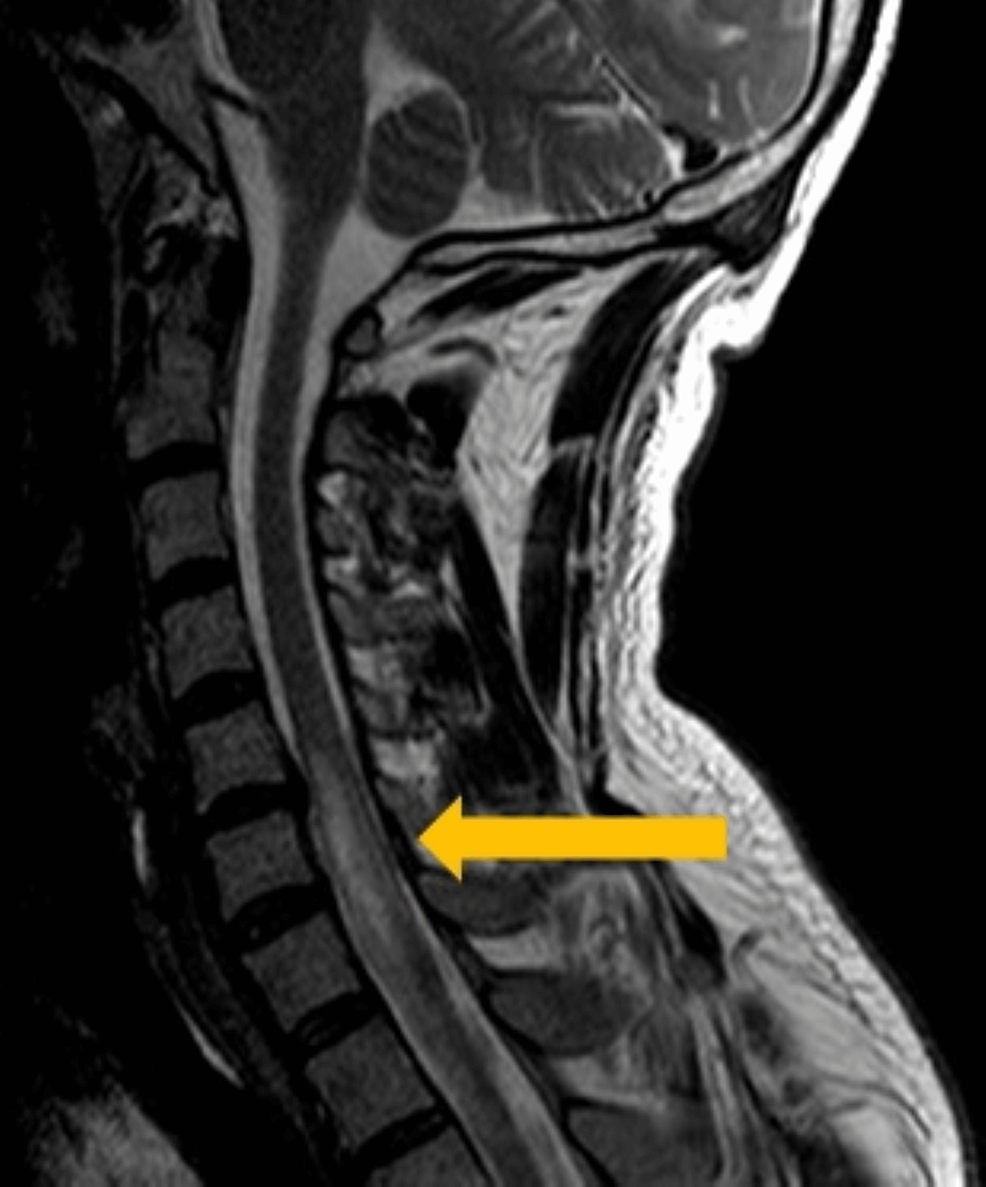
An etiological examination was performed. Blood tests specific to the case eliminated hypercoagulable and autoimmune disorders in the cytoplasmic antineutrophil and antinuclear antibodies, anticoagulants for lupus, Antiphospholipid and antinuclear antibodies are all negative S proteins, C protein fibrinogen, antithrombin III as well as VIII factor were in good condition as well as prothrombin gene, and Leiden factor mutations were detected. Additionally, the blood lipid profiles were normal (total cholesterol of 171 mg/dL; high-density lipoprotein (HDL) cholesterol 28 mg/dL; low-density lipoprotein (LDL) cholesterol 95 mg/dL and triglycerides 237 mg/dL) Glycated hemoglobin was 5.5 5 %. The patient was identified prior to diagnosis as hypertensive, throughout his hospitalization, he maintained a regular blood pressure without the need for antihypertensive medication. The neuraxial magnetic resonance scan and the Cranioencephalic scan (MRI) (Figure 3.) confirm the diagnosis. It also revealed no abnormalities in the vascular system. The vertebral echo and carotid Doppler was performed, revealing regular permeability to the lumen with no atherosclerotic disorder. A transesophageal echocardiogram was used to rule out an ovale-like foramen that was patent, septum defects, or the presence of vegetations. During admission, the patient was electrocardiographically monitored for 72 hours with no evidence of arrhythmias.
While in hospital, he suffered from nosocomial pneumonia as a result of without respiratory problems, and had successfully been treated with antibiotics and had a improvements in his clinical condition. The patient began rehabilitation for bladder training because of persistent urinary retention following attempts to remove the vesical catheter, and also motor training due to quadriplegia of level D on the Asia Impairment Scale with C6 neurological level that has left dominance and a hand-grip impairment that made it difficult to grasp objects. He had no impairment to his proprioceptive sensitivities. The patient was released after 15 days in hospital and was referred to a rehabilitation center for functional and motor rehabilitation center.
The infarction of the spinal cord is frequently not recognized in the ED because of its low frequency [11. In a majority of cases, chest pains, non-specific symptoms may be the initial sign and, in these cases, it’s located to the site of the ischemic lesion. Bladder dysfunction can be seen in more than half cerebral strokes, however it is uncommon in medullary infarction. However when it occurs it is typically related to urinary retention [55.
Aortic aneurysms are among the most predisposing disorders as well as coagulopathies, venous blood clots and surgical procedures for aortic arteries [44. The primary cardiovascular risk factor believed to be related to this condition is atherosclerosis however, due to its low frequency, its exact nature is unclear [2,62. The condition has been described as an embolization case of the patent foramen ovale7. The classic risk factors like diabetes mellitus and hypertension are linked to more severe medullary injuries [22.
The development of symptoms typically happens within hours. In about 50percent of cases there is a biphasic ictus typically, it is a radiating pain that radiates between the shoulders precedes the acute or transient spinal cord symptoms. At the peak, symptoms may be a time that could be anywhere from 35-45 minutes up or up to 24 hours [22. The initial scans (CT scans or MRI) can be normal for a number of days [3,83.8.
There aren’t any guidelines regarding the treatment of medullary strokes. They must be treated as strokes of the cerebral cortex [22. Anticoagulants, antiplatelets when they are clinically justifiable and controlled heart risk factor are among the most common methods. Other methods may be needed and must be evaluated individually for example, steroids to decrease medullary edema or cerebrospinal fluid drainage. There aren’t any data from clinical studies that recommend using fibrinolysis for treatment [3,83-8].
The degree of the symptoms present is a prognostic indicator with an increased likelihood of being predictive in the long run [11. Young adults and males tend to have more severe symptoms, but they are more likely to recover quickly. Rehabilitation programs are generally associated with positive outcomes. Chronic pain and autonomic dysfunction are common in patients who are followed up [2,4].
A diagnosis for spinal cord infarction is extremely difficult due to its relatively low prevalence and the range of symptoms present upon admission. Biphasic ictus as well as normal initial imaging, such as in this instance, could be a factor in the delayed diagnosis and consequently, the treatment and management. Idiopathic manifestations are quite common, in spite of a long and extensive research.
Antiplatelets/anticoagulants, control of cardiovascular risk factors, and rehabilitation are the main strategies for management and follow-up in these patients. While it is a bit scary, this condition generally has a better long-term outcomes.

We understand how important it is to choose a chiropractor that is right for you. It is our belief that educating our patients is a very important part of the success we see in our offices.