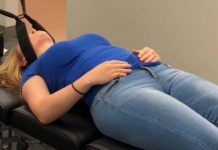
Is Walking Good For Sciatica Pain?
Walking is a surprisingly effective approach for relieving sciatic pain because regular walking spurs the release of pain-fighting endorphins and reduces inflammation. On the other hand, a poor walking posture may aggravate your sciatica symptoms.
Sciatica can be caused by a herniated disc, spinal stenosis, or Piriformis syndrome. Others find relief from sciatica pain by walking. This article discusses walking for sciatica pain treatment. Walking may be useful for sciatica sufferers. Resting or exercising to relieve discomfort has dangers.
Why is walking making my sciatica worse?
Walk with tiny, frequent steps. Lift using your legs and hips to maintain proper posture. If you have sciatica, see a doctor to rule out underlying issues. Too much speed can worsen the illness, so walk slowly.
Incorrect walking posture might compress lumbar discs. Leg length and walking speed must be assessed to discover if you’re causing discomfort or relieving symptoms. Focus on your breathing if you can’t walk or stand upright. This helps preserve proper posture and focus.
Compression of the lower back nerve causes sciatica. Nerve compression can weaken muscles. Ankle pain occurs. Standing tall helps sciatica. Try a standing desk if you can’t. Stretch your back and legs in addition to standing upright.
Is it better to rest or exercise with sciatica?
A physiotherapist may demonstrate gentle exercises for patients with sciatica. However, the correlation between imaging and symptoms is loose. Some exercises may effectively relieve the pain associated with sciatica, while others may worsen symptoms. If sciatica is affecting only one leg, rest is advised. If rest is recommended, patients can exercise after taking rest. An ice pack may also relieve the pain. Applying the ice pack to the affected leg and keeping it in place for 15 minutes may be good.
Although exercise may help with sciatic pain, patients should avoid exerting too much or performing strenuous exercises. Exercises should only be performed for five to ten minutes and gradually increase to a more rigorous routine. Avoid high-impact exercises like running or mountain biking until your symptoms have improved. During your exercises, try to stay focused and focus on your form. Breathing slowly will distract you from the pain. If you’re feeling discomfort, stop and talk to your healthcare provider. If the pain persists, they may recommend physical therapy.
How do I get my sciatic nerve to stop hurting?
There are several steps you can take to avoid sciatica pain when walking. When we walk on our toes, we put excessive pressure on the sciatic nerve and disk. To keep your spine in alignment, try to keep your head up and your chin level. A firm, level surface is also important. Even a slight incline can pressure the sciatic nerve, so avoid slick surfaces and sandy beaches. Do not skip your walking sessions because the pain will return.
Stretching your lower back is another key step. If your pain worsens when you sit, you should stretch your lower back. You should also avoid sitting for long periods, which can weaken the muscles and cause more pain. If the pain is severe, you should consult your healthcare provider before starting a stretching or aerobic exercise program. A physical therapist can help you with the proper stretching and strengthening exercises.
How much walking is good for sciatic pain?
To get started:
- Start by taking short walks.
- Increase your distance and intensity gradually.
- Walk for at least five minutes a day, and try not overdo it.
- Increase your pace gradually as your confidence grows.
Walking will strengthen your back and reduce pain. You can also take shorter walks if you don’t walk too fast. But keep in mind that walking faster will irritate your sciatic nerve and cause pain.
You can find ways to decrease your sciatica pain by taking walks. The sciatic nerve runs from the low back, through the gluteus maximus, and down the back of the leg. Several factors can irritate or pinch this nerve, including sitting for a long time, being overweight, or having type 2 diabetes. A simple way to reduce pain is to walk more. While walking is not a cure-all, it can help you get out of pain and stay active.
Before beginning an exercise program, you should follow your doctor’s recommendations. Avoid lifting objects heavier than 15 pounds or lifting them too far away from your body. If you are a heavy person, you should avoid elliptical machines. Also, avoid riding Peloton bikes. The higher the resistance, the more strain the sciatica is likely to cause pain. Depending on the severity of your sciatica, a doctor can give you specific instructions.
Is Climbing stairs good for sciatica?
Walking is beneficial for sciatica pain. While it can cause discomfort, the motion helps prevent further damage to the sciatic nerve. Climbing stairs and walking are both good for maintaining flexibility. In some cases, alternating between two types of OTC anti-inflammatories can also help. Patients should always consult with their doctors before starting a new exercise regimen. Walking in moderation can help prevent more damage to the sciatica nerve and help in maintaining a more comfortable lifestyle.
Depending on sciatica, you should avoid certain activities that worsen sciatica pain. The main reasons are lifting the leg from a lying position, walking, and climbing stairs. Walking on hard surfaces and lifting the leg from a squat can cause pain and stiffness. Physical trauma can result in fibrosis. Try to lead with your better side during walking, such as your heel.
Is bed rest good for sciatica?
While bed rest for acute sciatica can be effective for pain relief, it’s not recommended for long periods. While inactivity increases inflammation and resting in bed can aggravate symptoms, it’s still worth trying. Inactive rest is only good for a few days for pain relief, so you should plan to continue your normal activities and do light exercises. In some cases, a few days of rest to experience pain relief, but only if you have the symptoms and are not overly strained or dehydrated.
Traditional advice for treating sciatica involves total rest in bed, although recent studies said it could worsen symptoms. Experts recommend not sleeping in a bed for more than three days but recommend that patients take hot or cold packs several times a day. In addition to NSAIDs, acetaminophen and a few other medications may also help. Some people find that a firm mattress is the best way to manage sciatica.
How long will sciatica take to heal?
Sciatica can occur suddenly or gradually. The cause of sciatica can be anything from a herniated disk to arthritis in the spine. Sciatica is a common complaint, with 40% of American adults suffering from it. It is also one of the most common medical conditions, making it the third most common reason people see a doctor. It can also be caused by an injury, especially if the person has a lot of leg or back pain.
Pain associated with sciatica is often experienced in the lower back and radiates to the leg and hip. Depending on the severity and location, the pain may be mild or severe. A doctor can perform a sciatica MRI to rule out other causes of back pain. A doctor can also look at the condition by examining the piriformis muscle just below the hip. During the early stages, pain relievers, ice, or NSAIDs may be used on painful back areas to help alleviate the discomfort.
What is the Sciatica Symptoms?
Sciatica symptoms can be identified by the characteristic pain that travels from your lower back (lumbar region) to your buttock and then down the inside of your leg. You might feel the soreness practically anywhere along the nerve route, but it is most likely to follow a path from your low back to your buttock and the back of your thigh and calf. This is because your low back is the origin of the nerve pathway. The majority of cases of sciatica are brought on by issues that originate in the L4, L5, or S1 nerve roots. It’s most likely because a disc, bone, joint, or ligament is rubbing against the nerve, which can cause it to become compressed or irritated. Because of the inflammation that has developed due to the injury, the tissues and nerves now feel even more painful.
Will sciatica heal on its own?
There are many different ways to treat sciatic nerve pain, from anti-inflammatory drugs to spinal decompression surgery. Physical therapy is another common treatment option. However, this type of surgery requires several sessions and can be costly. Surgery is rarely recommended for sciatic pain and is usually reserved for severe cases. Instead, a simple exercise program like walking can help ease your symptoms and keep you active. However, you should take a few precautions to minimize the risk of sciatica and spinal stenosis.
If you have sciatica, it is best to start slow. Three miles per hour is a good starting place. While this is a reasonable pace, it’s important not to do it too quickly at first. Rather, start small, and increase your distance and time as your confidence grows. Walking is great for sciatica, so begin slowly and increase your time gradually. Walking is a great to experience pain relief, so don’t skip sessions just because it’s too painful.
Conclusion
Walking is good pain relief for sciatic nerve pain. The sciatic pain starts in the lower back pain and travels down to the sciatic nerve roots in your leg muscles. Orthopedic surgeons recommend exercise for sciatica for chronic back pain patients. Just gentle stretches, experience pain relief for all your pain conditions, and avoid sciatica pain. Physical therapy with a physical therapist is also recommended for this kind of pain.
Walking is good for sciatica because it improves your core muscles and lumbar spine. Just move at a slower pace to help relieve pain.

Doctor Osvaldo Pepa, Neurosurgery Service Physician at Hospital San Martin, La Plata, Argentina. I graduated last November 16, 1984 with a Medical Degree at the Universidad Nacional de La Plata. The Medical Board of La Plata, District 1, licensed me as a Neurosurgeon in 1990. I hold a Provincial and National License and an active member of the Neurosurgery Society of La Plata, World Ozone Therapy Federation, and Inter American Society of Minimally Invasive Surgery.