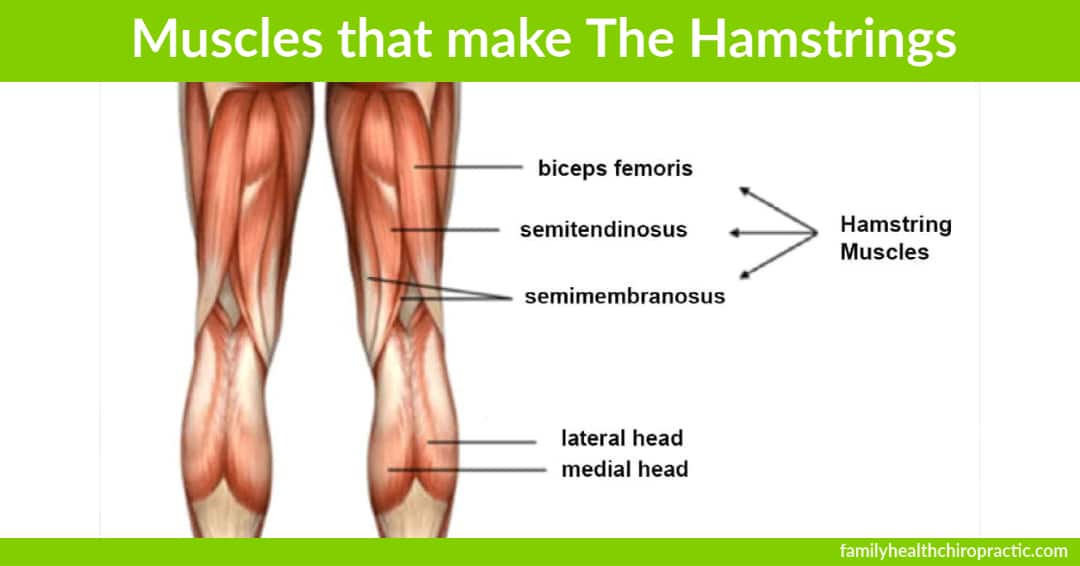

What to Know About Tight Hamstrings Almost every patient that we evaluate for back pain in our chiropractic office has...
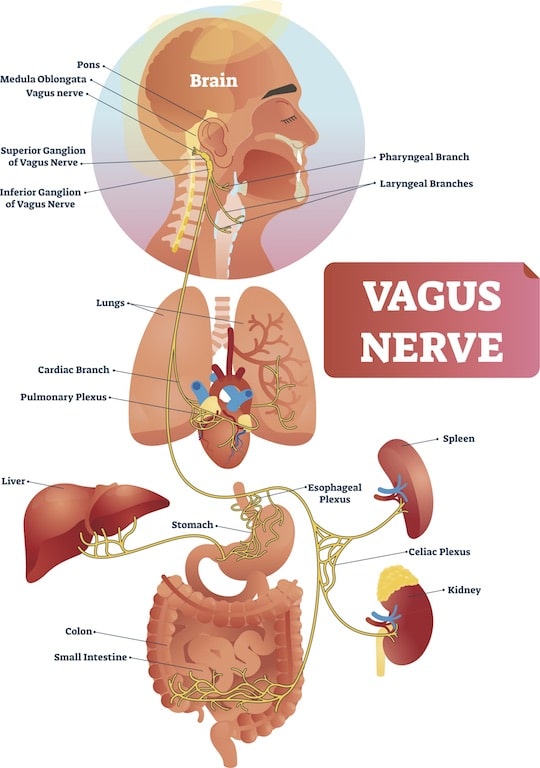


With each passing year, more and more evidence is mounting supporting the benefits of regular chiropractic adjustments. Every year, scientists are publishing scientific chiropractic-based studies aimed...
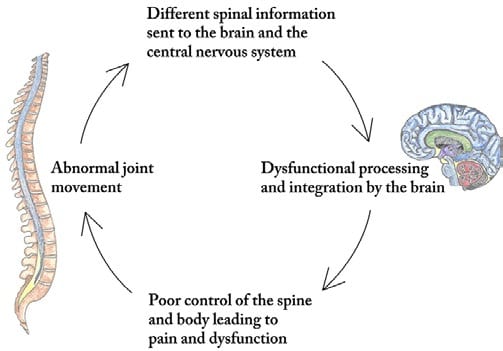


Should I See A Chiropractor? Every year, Millions of people in the U.S. see chiropractors for relief ofheadaches; back pain, shoulder, foot and neck pain. People...



Do you ever ask yourself why your neck is so stiff, or why you have that nagging headache that doesn’t seem to want to go away?...


The post Avoiding Back Pain while Shoveling and stretches for when you are done. appeared first on Active Family Chiropractic Blog.