The first randomized controlled study testing the efficacy of a short course opioids for acute nonspecific neck/low back pain suggests that opioids do not relieve acute neck or low back pain in the short-term and can lead to worse outcomes over the long-term.
After 6 weeks there was no significant difference between the pain scores of patients taking opioids and those who took a placebo. After one year, the pain scores of patients who received placebos were slightly lower. After 1 year, opioid users were also at a higher risk of opioid abuse.
Senior author Christine Lin, Ph.D., from the University of Sydney told Medscape Medical News that this is a “landmark trial” with “practice changing” results.
Lin explained that “we did not have any good evidence before this trial on whether opioids are effective for acute neck or low back pain, but opioids are one of the most commonly prescribed medicines for these conditions.”
Lin stated that based on these results “opioids shouldn’t be recommended at any time for acute neck and low back pain,”
The results of the OPAL study have been published online in The Lancet on June 28.
Rigorous Test
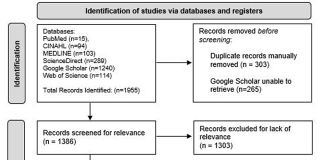
The trial was conducted at 157 primary care and emergency departments in Australia, with 347 adults who experienced low back pain or neck pain for 12 weeks or less.
They were randomly allocated (1:1) to receive guideline-recommended care (reassurance and advice to stay active) plus an opioid (oxycodone up to 20 mg daily) or identical placebo for up to 6 weeks. Naloxone is given to prevent opioid-induced constipation, and to improve blinding.
The primary outcome was the pain severity at six weeks, as measured by the pain severity subscale (10-point scale) of the Brief Pain Inventory.
After 6 weeks of opioid therapy, there was no difference between placebo and opioid therapy in terms of pain relief or functional improvement.
The mean pain score was 2.78 for the opioid group at 6 weeks, compared to 2.25 for the placebo group. (Adjusted median difference, 0.53, 95% CI -0.00 – 1.07, P=.051). At 1 year, the mean pain scores of the placebo group were lower than those of the opioid group (1.8 and 2.4).
The risk of opioid misuse was doubled at 1 year for patients randomly assigned to receive opioid therapy during 6 weeks as compared to those randomly assigned to receive placebo during 6 weeks.
At 1 year, the Current Opioid Use Measure (COMM), a scale that measures current drug-related behavior, indicated that 24 (20%) patients from 123 patients who received opioids, were at risk for misuse. This was compared to 13 (10%) patients from 128 patients in a placebo group ( p =.049). The COMM is a widely-used measure of current aberrant drug related behavior among chronic pain patients who are prescribed opioid therapy.
Results Raise “Serious Questions”
Lin told Medscape Medical News that “I think the findings of the research will need to be distributed to doctors and patients so they receive the latest evidence on opioids.”
“We must reassure doctors and their patients that the majority of people with acute neck and low back pain recover well over time (normally within 6 weeks). Therefore, management is simple – stay active, avoid bed rest and, if needed, use a heat pack to relieve short term pain. Consider anti-inflammatory drugs if drugs are needed,” Lin added.
The authors of the linked comment state that the OPAL trial raises serious questions regarding the use of opioids for acute neck and low back pain.
Mark Sullivan, MD PhD, and Jane Ballantyne MD, from the University of Washington in Seattle, note that clinical guidelines recommend opioids to patients with acute neck and back pain when other drugs fail or are contraindicated.
As many as two thirds of patients may receive an opioid for back or neck pain. Sullivan and Ballantyne say that it is time to reexamine these guidelines.
The National Health and Medical Research Council (NHMRC), the University of Sydney Faculty of Medicine and Health (University of Sydney Faculty of Medicine and Health) and SafeWork SA funded the OPAL study. The authors of the study have not disclosed any relevant financial relationships. Sullivan and Ballantyne have served as board members of Physicians for Responsible Opioid Prescribing (unpaid), and paid consultants for opioid litigation.
Lancet. Online published June 28, 2023. Abstract
Join us on Facebook or Twitter for more Medscape Neurology News.

We understand how important it is to choose a chiropractor that is right for you. It is our belief that educating our patients is a very important part of the success we see in our offices.