Editor’s note: Get inspired with a weekly roundup of simple tips for living well. Sign up for CNN Life, But Better to receive information and tools that will improve your well-being.
CNN
A new study suggests that opioid medications may not be effective in treating low back pain, despite being one of the most commonly prescribed treatments.
It is not uncommon to experience pain in the lower back and neck. According to a study of data from the Global Burden of Disease Study, neck pain is the fourth most common cause of disability in the world.
According to the North American Spine Society, chronic low back pain is defined by symptoms lasting more than 12 week.
The clinical guidelines of the society state that physicians should limit opioid use to a short period when treating this type of pain. The use of opioids for pain relief is only recommended when other pharmacological treatment has failed or if the patient cannot take them due to personal reasons.
In a press release, Christine Lin, professor at the Institute for Musculoskeletal Health of the University of Sydney, Australia, said that despite these guidelines, “there is no evidence of their effectiveness in reducing pain,” opioid pain relievers were still prescribed for people suffering from lower back and neck discomfort in many countries. Lin is the senior author of a study published in The Lancet on Wednesday.
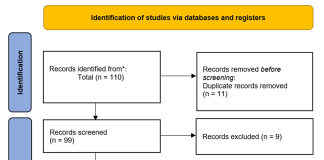
A small group of 310 patients was studied by the scientists due to the lack of research. Patients in Sydney sought treatment for neck or lower-back pain at primary care clinics and hospitals between February 2016 to March 2022. Participants were averagely 44 years old at the start of the study and had suffered from neck or lower back pain for 12 weeks.
The participants were randomly divided into two groups. One group received a combination of up to 20 micrograms per day of the opioid oxycodone. Naloxone was used as a way to prevent constipation – a common side-effect of opioids – and keep participants from knowing which group they were. The other group was told to take a pill that contained a placebo.
Both groups received care tips from the doctor, whom they were instructed to visit weekly. The doctor reassured them and advised them to avoid bed rest, stay active and, if necessary, avoid other treatments, including nonopioids.
The authors found that opioids were no more effective than placebos in treating back and neck pain. Six weeks after treatment, the average pain score in the opioid group was 2.78 and 2.25 in placebo group. This difference increased over time. The opioid group reported more ongoing pain in weeks 26 and 52 compared to the placebo group.
The authors also discovered opioids are unlikely to relieve back and neck pain but they may also cause harm, even after short-term use.
The opioid group scored lower on mental health and had more reports of nausea and dizziness than the placebo group. Lin stated in a press release that “we also know that even a short-term prescription of opioid pain relievers increases the risk of long-term opioid misuse.”
Opioids and pain
Experts and authors of the study who were not involved in the new study have theories as to why opioids didn’t prove more effective than placebo.
Experts said that it is possible that the opioid group’s back or neck pain had more underlying causes than the authors realized — factors that are known to be resistant to opioid treatment.
According to Dr. Mark D. Sullivan, and Dr. Jane C. Ballantyne who were not involved in the study, the pain treated could have been chronic, recurring, rather than the type of pain caused by acute injury. Sullivan is a Professor of Psychiatry and Behavioral Sciences, and Ballantyne, a retired Professor of Anesthesiology, Pain Medicine, and the University of Washington.
Sullivan and Ballantyne stated that participants only had to be pain-free for 1 month before they experienced their current episode. “If many of these patients had recurrent back pain, that could explain the non-response.” Low back pain is reported to change over a period of a year.”
Dr. John Finkenberg is a San Diego-based orthopedic spine surgeon who believes that certain areas of neck and back pain need to be treated separately. He was not involved in the study.
“If someone had both going on, they will, quite frankly, have a systemic issue going on. Whether it is general arthritis or rheumatoid. We have to be cautious with patients who come in with both,” said Finkenberg, also the president of the North American Spine Society.
The authors did not collect data on the care that doctors provided in follow-up visits, so they were unable to determine whether patients followed advice or if it had any impact. Only 57% of participants indicated that they took their medication as prescribed. Just over half of those participants took more than 80% their prescriptions.
Back and neck pain: How to manage it
The authors believe that because opioids are not beneficial but can cause harm, they shouldn’t be prescribed for acute neck or lower-back pain.
Lin stated in the news release that doctors should instead be encouraged to focus their attention on patient-centred methods, which could include advice about staying active and simple pain relievers. “The good news for people with acute neck and low back pain is that they recover naturally within six weeks.”
The authors studied nonspecific neck or back pain, which is pain that has an unknown cause. Finkenberg argued that when doctors don’t have a clue as to the cause, they shouldn’t use opioids as a first option or a quick solution.
Nonsteroidal anti-inflammatory medications, or NSAIDS, such as ibuprofen naproxen and Celecoxib, are helpful alternatives to opioids. According to a study conducted in February, a combination of an NSAID with a prescription muscle relaxing drug can reduce pain and disability in a week.
Exercises that improve range of motion can also be helpful. Stretches can be used to improve or maintain mobility.
Finkenberg advised that people with these pains “should also use their body as a barometer.” Don’t force yourself to continue an activity if your body is uncomfortable. This could cause the area to become more inflamed, causing further pain and damage.
Finkenberg advised that if your pain or weakness persists after three to four week, you should “really go to a specialist as it is difficult to detect these subtleties of why people are experiencing discomforts.” If advanced diagnostic tests are required, it is better to get them sooner.

We understand how important it is to choose a chiropractor that is right for you. It is our belief that educating our patients is a very important part of the success we see in our offices.