In the moments before her life was shattered, Megan Freedman had attended an unforgettable business dinner attended by beloved colleagues at a fashionable dining establishment located in Santa Monica, Calif. which overlooked the Pacific Ocean.
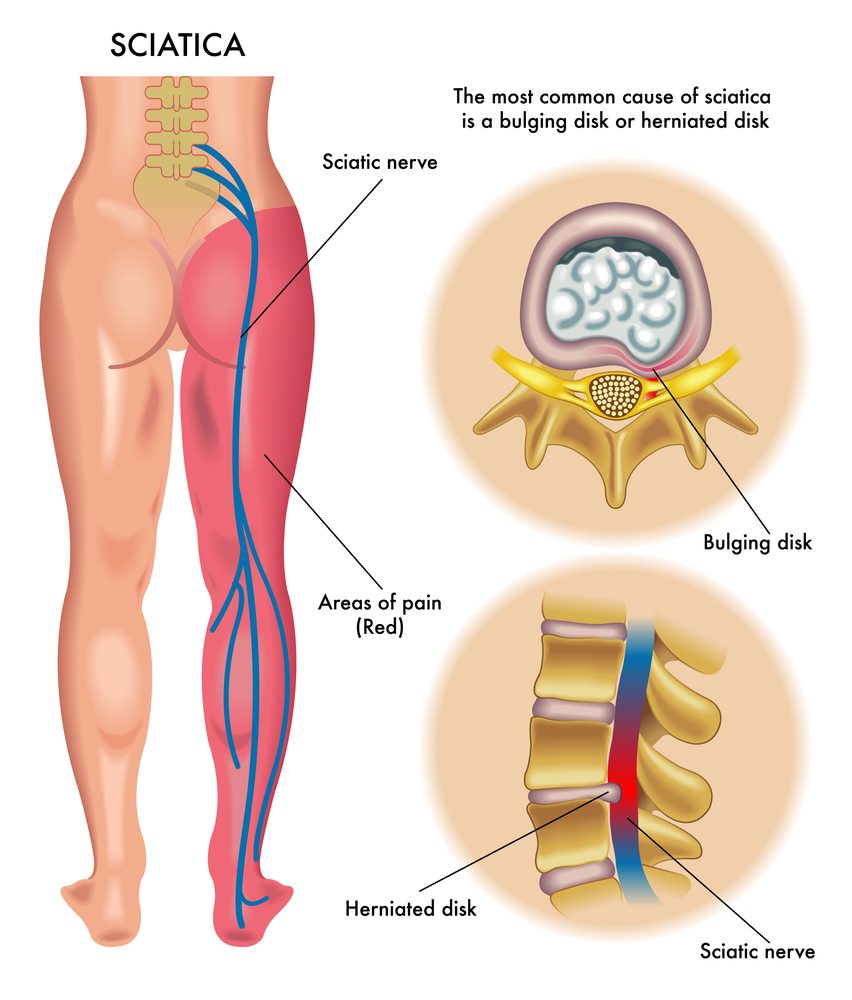
Sciatica
She was confronted by a raging leg pains that struck her without warning. The Washington Post

“We’d enjoyed the most,” recalled Freedman, the proprietor of the New York City fashion showroom who visited Los Angeles in October 2019 to meet her designers and buyers from national retailers. The wall was hung up in the back of the restaurant, after the meal, Freedman was chatting as she and her companions stood in line for their vehicles. As she got up, her left foot was suddenly swollen which caused her to fall. “I was not drinking,” she said. “I had just gone boink and somebody had to help carry me up.”
The next day, Freedman awoke to stabbing pains in her leg, which was partially numb. “I was absolutely certain I was suffering from a herniated disk,” she recalled. Freedman had spent the last couple of days “lifting boxes” and transporting” heavy suitcases packed with samples of clothing to appointments. A few years ago, she was suffering from similar type of pain on her arm to the left, caused through two discs herniated that were in her neck.
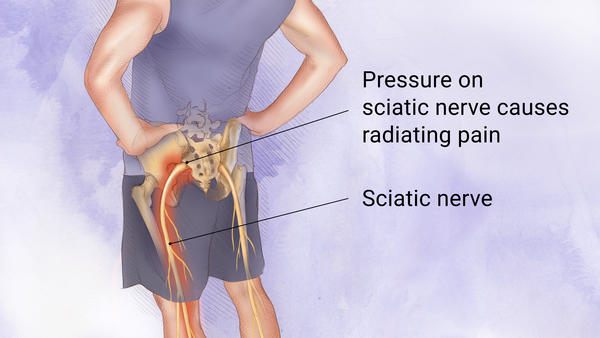
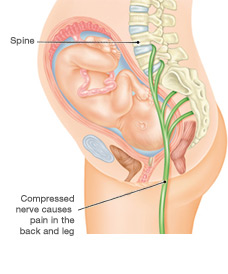
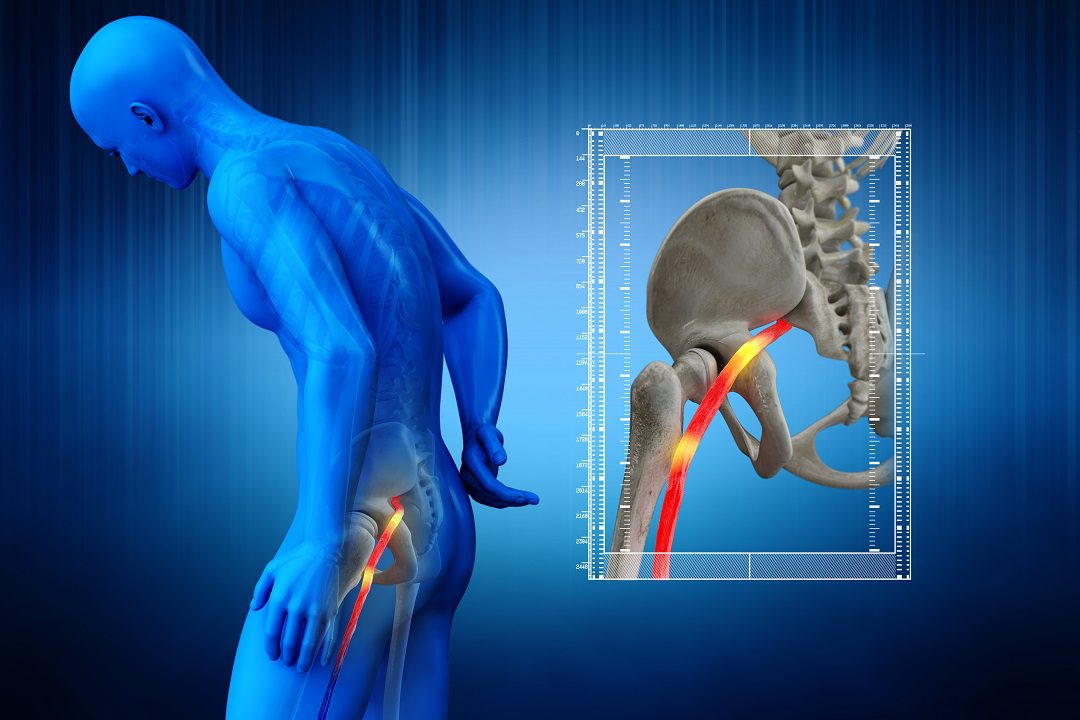
“I suspected I was suffering from sciatica,” she said in reference to leg pain which radiates from the knee. It is typically caused by disk or bone spur that presses against the sciatic nerve.
Freedman was to spend for the following eight weeks running between doctor’s offices and emergency rooms throughout Los Angeles and Manhattan in what she described as “ridiculous” suffering. Her leg was frequently so weak that she needed to raise it using her hands.
In December, just moments before she was discharged from the New York hospital after a nine-day hospital stay, Freedman learned she had an illness of serious severity that had been developing without prior warning.
“I come from a lineage that is full of heart diseases or cancer” told Freedman, 54. “I had no idea that this would happen to me.”
Crying on the flight
Incredulous at the intensity of her pain and the difficulty walking, the person who Freedman was staying took her to the emergency department of an Los Angeles teaching hospital. Doctors at the hospital were also suspicious of sciatica and prescribed the painkiller narcotic Dilaudid. If she was not better within three days they recommended to return back.
Freedman was not able to recover and she fell multiple times. She was taken to an ER and had an MRI scan of her lower spine and did not reveal anything concerning. Doctors recommended a stronger opioid, which she stated barely eased the discomfort. A few days later, she took a flight back in New York. “I just sat weeping on that plane,”” Freedman recalled.
She saw her Manhattan orthopedist that she had visited for neck problems. He examined the MRI and also took X-rays. Unable to pinpoint what might cause the problem, he suggested Freedman to an spine specialist. The specialist was confused and so was a second spine orthopedist. The doctor provided her with one of the epidural injections of steroid in her lower back but neither of them relieved discomfort, she recommended that she consult an neurologist.
Freedman remembers feeling a growing feeling of despair over her constant pain and lack of an explanation.
The neurosurgeon recommended an electromyography exam and an electromyography test and a nerve conduction study to assess the operation of nerves as well as muscle in the leg of Freedman. The results suggested it was coming from her front pelvis, not from her spine. In the event that she had blood clots or peripheral artery disorder, where the veins narrow due to the buildup of plaque which restricts the flow of blood, he requested an ultrasound scan of her left leg from the groin, and also the CTA scan, which checks blood vessels for abnormalities.
A Sunday morning, a few days prior to the tests being set, Freedman headed for the ER of the Manhattan teaching hospital, to the neurologists.
“I could not bear the pain anymore,” she recalled. After waiting for a while, the patient was transported to an examination room where she was told an experienced doctor said that the ER personnel was awash with “bigger fish to catch” and suggested she go home. Freedman doesn’t know what provoked his comment, but that he believed she was suffering from sciatica and required rest.
An unpleasant encounter
“That was the most painful moment of my life,”” she admitted, crying at the thought. “Being being told that there’s no problem with you and you shouldn’t worry about it. I was so embarrassed.”
After that, Freedman went to the ER at Mount Sinai, the teaching hospital where she’d been consulting a neurologist for a few years to manage chronic migraines.
The treatment was not as pleasant. Doctors admitted her, and teams from different specialties including neurology, oncology and rheumatologywere ordered to conduct tests to determine the cause of Freedman who was given the nickname of “the strange legs lady.”
Initially, doctors focused an area on her ovary, which was described as “concerning” but it was later deemed to be harmless. The “highly unusual” thyroid lump was also dismissed. Doctors observed that Freedman’s leg strength increased following a course of steroids, and she could walk but her pain remained constant and extremely. Sciatica was ruled out and scans revealed only mild spinal degeneration.
Freedman’s EMG and nerve conduction tests were not normal and an MRI revealed the left femoral nerve one of the biggest nerves in the leg which regulates movement and senses pain.
Doctors were concerned that her chronic thyroid problems and the improvement in her thyroid function on steroids indicated an autoimmune condition where the body accidentally attacks itself. They started exploring the possibilities. Positive blood tests for PR3 that detects antineutrophilcytoplasmic antibodies (ANCA) which is a protein that is mistakenly attacking the healthy white blood cells has greatly limited the possibilities.
The day before Freedman’s discharge, a group of rheumatologists came into her room to inform her that they suspected she was suffering from polyangiitis granulomatosis (GPA) which was previously called Wegener’s disease. GPA is a type of vasculitis, which is an inflammation of blood vessels that may cause damage to organs. The condition is often affecting the kidneys, lungs , and sinuses.
GPA that mimics an infection, can manifest in a flash or over the course of months or weeks. The severity and signs vary based on the organ involved. Treatment can include high doses corticosteroids, typically in conjunction with other powerful drugs to reduce your immune system. If treated in the early stages it is possible to recover fully If not treated, GPA can be fatal.
A ‘typical presentation’
At the start of his professional career, in late 70s Anthony S. Fauci who was the long-standing Director of the National Institute of Allergy and Infectious Diseases along with his colleagues discovered the cause of the disease, which in the early 1970s killed the majority of people in less than two years. Fauci also played a role in the development of a the treatment of GPA that is 95 percent effective.
In the case of Freedman the disease impacted the femoral nerve. “It was an unusual manifestation,” said Weiwei (Wendy) Chi, the Mount Sinai Rheumatologist who has been treating Freedman since her diagnosis. Freedman also suffered from nosebleeds and sinusitis. These could be signs that indicate GPA.
The patient immediately started taking steroids in high doses that helped improve the ability of the leg, but didn’t help to reduce the pain. The injury in her femoral nerve is likely to last forever. The medications commonly prescribed to treat her pain been effective, Chi said, so “she’s using opioids for the moment.”
“The most confusing aspect of her situation is the constant pain” which is persistent and unabated, Chi observed. “I am not a fan of giving chronic opioids , but we’ve tried everything else and nothing has did anything to help.”
The 2 1/2 years that followed Freedman’s diagnosis were rough. She was hospitalized multiple times for acute pancreatitis. which is a painful and serious irritation of the pancreas, which is usually due to gallstones. She contracted coronavirus through her hospital roommate during a stay. On May 20, 2021 Freedman was operated on to eliminate her gallbladder.
Her company of 20 years dissolved due to the pandemic. Freedman stated the company was forced to shut down her showroom and cut off her employees of five; she has since moved to a home office.
Because her entire life is dependent on a set of medications that weaken your immune system the coronavirus is an increased chance. There was no protection from the two initial doses of vaccine because the body didn’t produce antibodies.
As the omicron waves swept across New York City in late 2021, Freedman decided she could not take the risk of living in the city with her family, that includes a son who is who is in high school. She moved to a tiny town in the Cali’s Coachella Valley near her brother before returning home to New York two months ago. (She received covid-19 as well during January.)
In California she was treated with injections of Evusheld which is an experimental drug specifically designed for patients with immunocompromised. Doctors believe she may have acquired antibodies following the administration of an additional coronavirus vaccine in April, following the return trip back to New York.
Prior to GPA her health was good. “This disease is very scary and really shook in my butt” the woman said. “Not everyone is aware about it, and a lot of people sufferers have serious instances.”
Freedman “has been fairly stable over the last 3 years,”” Chi said. Chi, who described the extent of her condition to be “in mid-range. She doesn’t suffer from an organ that is life-threatening, such as rapid renal failure.”
“In extreme cases, individuals can be healthy one day, and be within the ICU the next day,” the rheumatologist said. “It’s so unpredictable.”
Submit your solved medical mystery to [email protected]. Do not submit unsolved cases. Read previous mysteries at wapo.st/medicalmysteries.